Dengue NS1 vs IgM vs IgG: Which Test Should You Use and When?
The answer is straightforward: NS1 tests are best for early detection, IgM indicates recent infection, and IgG helps identify past or secondary infection. Understanding dengue NS1 vs IgM vs IgG is essential for selecting the right diagnostic method at the right time and improving clinical outcomes.
What Is Dengue and Why Testing Timing Matters
Dengue is a mosquito-borne viral infection that affects millions of people annually, particularly in tropical and subtropical regions. Its symptoms—such as fever, headache, and muscle pain—often overlap with other viral illnesses, making laboratory testing critical for accurate diagnosis.
Timing plays a decisive role in dengue diagnostics. The viral antigen and the body’s immune response appear at different stages of infection, which directly impacts test selection. Misjudging timing may lead to false-negative results or delayed diagnosis.
This is why understanding the appropriate testing window versus antibody-based testing is crucial in clinical practice. Proper timing ensures optimal dengue test accuracy NS1 vs IgM and improves patient management.
In endemic regions, dengue diagnosis is further complicated by overlapping circulation of other arboviruses such as Zika and chikungunya. This increases the risk of misdiagnosis when relying solely on clinical symptoms.
Laboratory confirmation therefore becomes essential not only for individual patient care but also for public health surveillance. Accurate identification of dengue cases supports outbreak monitoring and resource allocation, making appropriate test selection a critical component of healthcare systems.
Dengue NS1 Test: Early Detection of Acute Infection
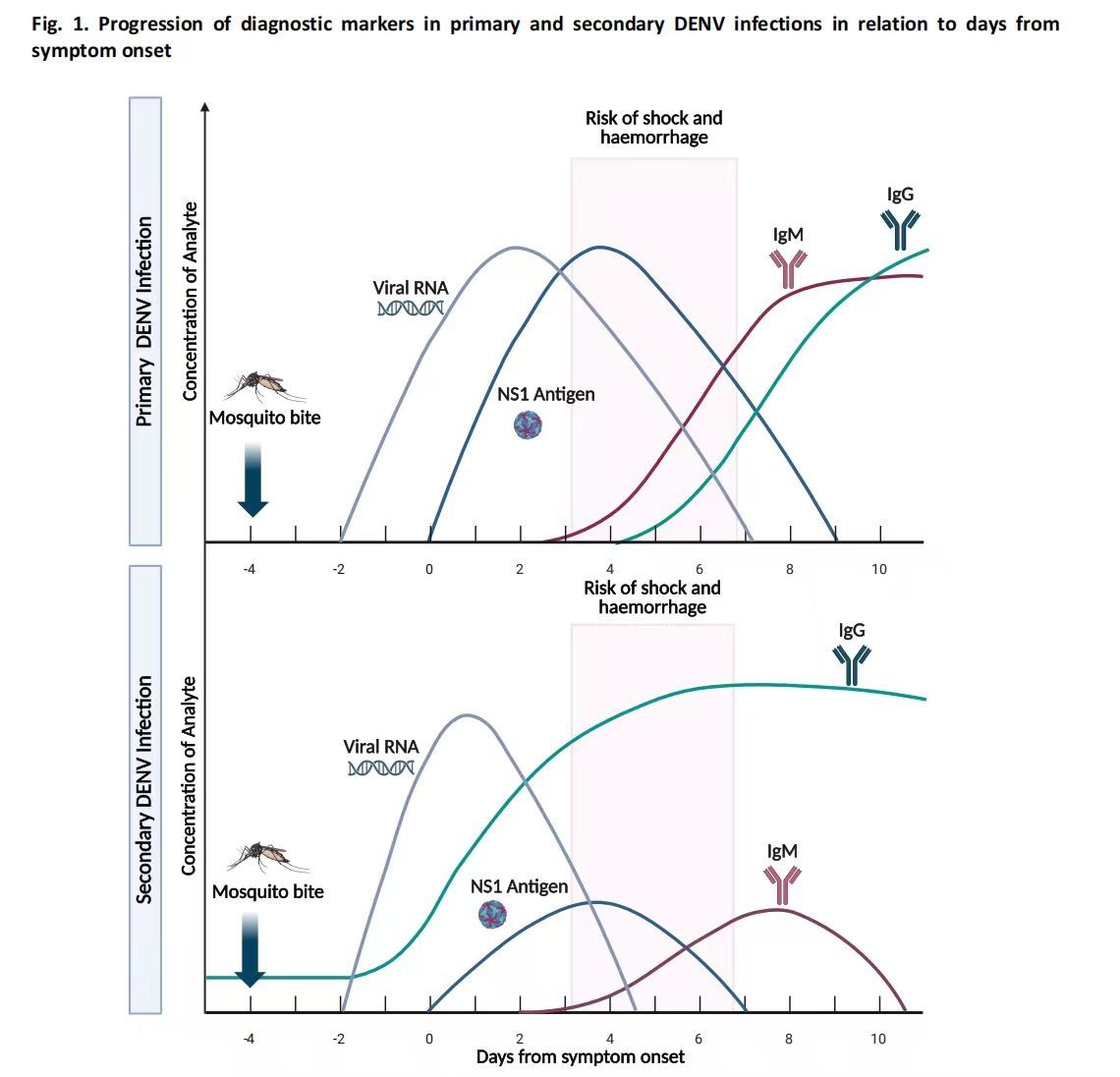
The NS1 antigen is a viral protein released into the bloodstream during the early phase of infection. In primary dengue infections, NS1 antigen is generally detectable for a longer period, often up to nine days after symptom onset. In secondary infections, however, NS1 detection may decline earlier because pre-existing antibodies can form immune complexes with circulating NS1 antigen.
This means that NS1-based testing is typically more sensitive during primary infection, while secondary dengue cases may require additional antibody testing for accurate diagnosis.
NS1 testing is particularly useful in identifying acute dengue infections before the immune system produces detectable antibodies. This early detection allows clinicians to initiate monitoring and supportive care promptly.
Among these three diagnostic markers, NS1 stands out for its role in the initial stage. However, its sensitivity may decrease as the infection progresses, especially in secondary infections where antibody response is faster.
From a clinical perspective, understanding the difference between antigen and antibody detection in dengue testing helps avoid relying on NS1 beyond its optimal detection window.
It is also important to note that NS1 detection performance may vary depending on viral load and patient immune status. In primary infections, NS1 levels are typically higher and more detectable, while in secondary infections, rapid antibody responses may reduce circulating antigen levels.
This variability highlights the importance of combining NS1 with antibody testing in certain clinical scenarios to improve overall diagnostic confidence.
Dengue IgM Test: Detecting Recent Infection
IgM antibodies are produced by the immune system shortly after infection, usually becoming detectable around day 4 to day 7. They indicate a recent or ongoing infection.In primary infections, IgM antibodies usually become detectable between days 3–5, peak around two weeks, and gradually decline over the following months. In secondary dengue infections, IgM responses are often weaker and may even be absent in some patients.
Because of this difference, relying solely on IgM testing in suspected secondary dengue cases may lead to false-negative interpretations.
Compared with NS1, IgM testing is more useful in the later phase of the acute stage. It is often used when patients present after the initial days of symptoms.
When analyzing these three markers, IgM fills the diagnostic gap after NS1 detection declines. However, IgM may persist for weeks, which can complicate interpretation in endemic areas.
Therefore, understanding when to use NS1 dengue test versus IgM is essential for accurate diagnosis and avoiding misinterpretation of results.
Additionally, IgM results should always be interpreted alongside clinical history and epidemiological context. In regions with frequent dengue exposure, residual IgM antibodies may persist longer than expected, potentially leading to false assumptions about recent infection.
This reinforces the need for a structured diagnostic approach when evaluating suspected dengue cases.
Dengue IgG Test: Identifying Past or Secondary Infection
IgG antibodies develop later in the infection, typically after day 7, and can persist for months or even years. Their presence indicates past exposure or secondary infection.The timing of IgG response differs significantly between primary and secondary dengue infections. In primary infection, IgG appears relatively late and persists long term. In secondary infection, IgG rises rapidly during the early phase and often becomes the dominant antibody response.
Early high IgG levels together with positive NS1 or RNA findings strongly suggest secondary dengue infection and may indicate a higher risk of severe disease.
In secondary dengue infections, IgG levels rise rapidly and can appear earlier than IgM. This pattern is important because secondary infections are often associated with higher risk of severe disease.
In the context of these three markers, IgG plays a key role in epidemiological assessment and risk stratification. It also helps distinguish between primary and secondary infections.
The difference between NS1 and IgM dengue testing becomes even more significant when IgG is included in the diagnostic strategy.
The presence of IgG is particularly relevant in assessing the risk of severe dengue. Secondary infections associated with different serotypes can trigger more intense immune responses, increasing the likelihood of complications such as dengue hemorrhagic fever.
Therefore, IgG testing is not only useful for retrospective diagnosis but also for clinical risk assessment.
What are the Key Differences between NS1, IgM and IgG?
Detection Target and Timing
NS1 detects viral antigen, while IgM and IgG detect the immune response. NS1 appears early, IgM appears in the intermediate phase, and IgG dominates later.
Clinical Interpretation
NS1 positivity indicates active infection. IgM suggests recent infection, while IgG indicates past exposure or secondary infection.
Primary vs Secondary Dengue Infection
| Marker | Primary Infection | Secondary Infection |
|---|---|---|
| NS1 Antigen | Detectable longer, up to ~9 days | Declines earlier due to immune complexes |
| IgM Antibody | Strong response, peaks around 2 weeks | Lower or sometimes absent |
| IgG Antibody | Appears later | Rises rapidly and dominates early |
| Diagnostic Challenge | Easier early NS1 detection | Higher risk of false-negative NS1/IgM |
When to Use Each Dengue Test
Choosing the right test depends on symptom onset and clinical scenario.
- Days 1–5: NS1 test is preferred for early detection
- Days 5–10: IgM testing becomes more reliable
- After Day 7: IgG helps identify past or secondary infection
In suspected secondary dengue infections, clinicians should be cautious when interpreting isolated NS1 or IgM results. Combination testing strategies that include NS1, IgM, and IgG markers are often more effective for identifying different immune response patterns across infection stages.
In real-world clinical settings, patient presentation does not always follow textbook timelines. Delayed consultation or unclear symptom onset may complicate test selection.
In such cases, relying on a single marker may not provide sufficient diagnostic clarity. A combined testing approach helps mitigate uncertainty and ensures more comprehensive evaluation across different stages of infection.
In practice, combining these tests often provides the most accurate diagnosis. Understanding the different dengue testing markers ensures that clinicians use the right tool at the right time.
This approach also improves overall dengue test accuracy NS1 vs IgM, especially in regions with high dengue prevalence.
Can One Test Detect All Stages?
Single-marker testing has limitations because each marker is only detectable during a specific phase. This is where combination testing becomes highly valuable.
From a workflow perspective, combination testing also reduces the need for multiple sample collections and repeat visits. This not only improves patient experience but also enhances operational efficiency in busy clinical environments.
For healthcare providers in dengue-endemic regions, adopting integrated testing strategies can significantly improve both diagnostic speed and resource utilization.
A Dengue IgG/IgM and NS1 Combo Rapid Test enables simultaneous detection of viral antigen and antibodies from a single sample. This approach covers multiple stages of infection, reducing the risk of missed diagnoses.
For example, a well-designed combo test can detect NS1 for early infection while also identifying IgM and IgG for later stages. This integrated approach simplifies clinical workflows and improves diagnostic confidence.
Medotex’s dengue combo rapid test is based on a chromatographic immunoassay that delivers results in approximately 15 minutes. It supports detection of NS1 antigen as well as IgM and IgG antibodies using whole blood, serum, or plasma samples.
Clinical performance data indicate high sensitivity and specificity for NS1 and IgM detection, ensuring reliable results in real-world settings. This makes combination testing a practical solution in primary care, hospitals, and dengue-endemic regions.
Conclusion
Understanding dengue NS1 vs IgM vs IgG is essential for accurate diagnosis and effective patient management. Each test plays a distinct role depending on the stage of infection, and incorrect timing can significantly impact results.
By combining antigen and antibody detection, clinicians can achieve more comprehensive and reliable diagnostics. For healthcare providers seeking efficient and scalable dengue testing solutions, manufacturers such as Medotex offer practical options to support timely diagnosis and improved clinical outcomes.